Epilepsy Surgery: Modern Imaging, Operative Electroencephalography, and Laser Navigation in the Fight Against Epilepsy
Epilepsy affects approximately 1% of the world’s population and occurs across all age groups. The quality of life of affected patients is often significantly impaired. Despite treatment with antiepileptic medications, about one third of patients do not achieve seizure freedom. In such cases, epilepsy surgery represents a therapeutic option whose effectiveness has been clearly demonstrated in recent years.
There are long-standing and close collaborations with the Epilepsy Monitoring Units of the University Clinic for Pediatrics and Adolescent Medicine (Ao. Univ.-Prof. Dr. med. univ. Martha Feucht), the University Clinic for Neurology (Ao. Univ.-Prof. Dr. med. univ. Ekaterina Pataraia), the University Clinic for Radiology and Nuclear Medicine, and the Neurological Rehabilitation Center Rosenhügel (Univ. Prof. Dipl. Ing. Dr. med. Christoph Baumgartner). In keeping with an interdisciplinary approach, complex cases are discussed at monthly conferences within the Epilepsy Surgery Board and the Pediatric Epilepsy Board.
A dedicated specialized outpatient clinic for epilepsy surgery also enables highly specialized care for all epilepsy surgery patients, both preoperatively and during long-term follow-up.
In invasive diagnostics, the treatment of epilepsy patients may involve the implantation of subdural electrodes as well as stereotactic and navigation-guided depth electrodes. Therapeutic procedures include standard resective techniques, awake surgery, multilobar disconnections, hemispherotomy, callosotomy, vagus nerve stimulator implantation, and deep brain stimulation.
The fundamental goal of epilepsy surgery is postoperative seizure freedom without causing unacceptable neurological deficits.
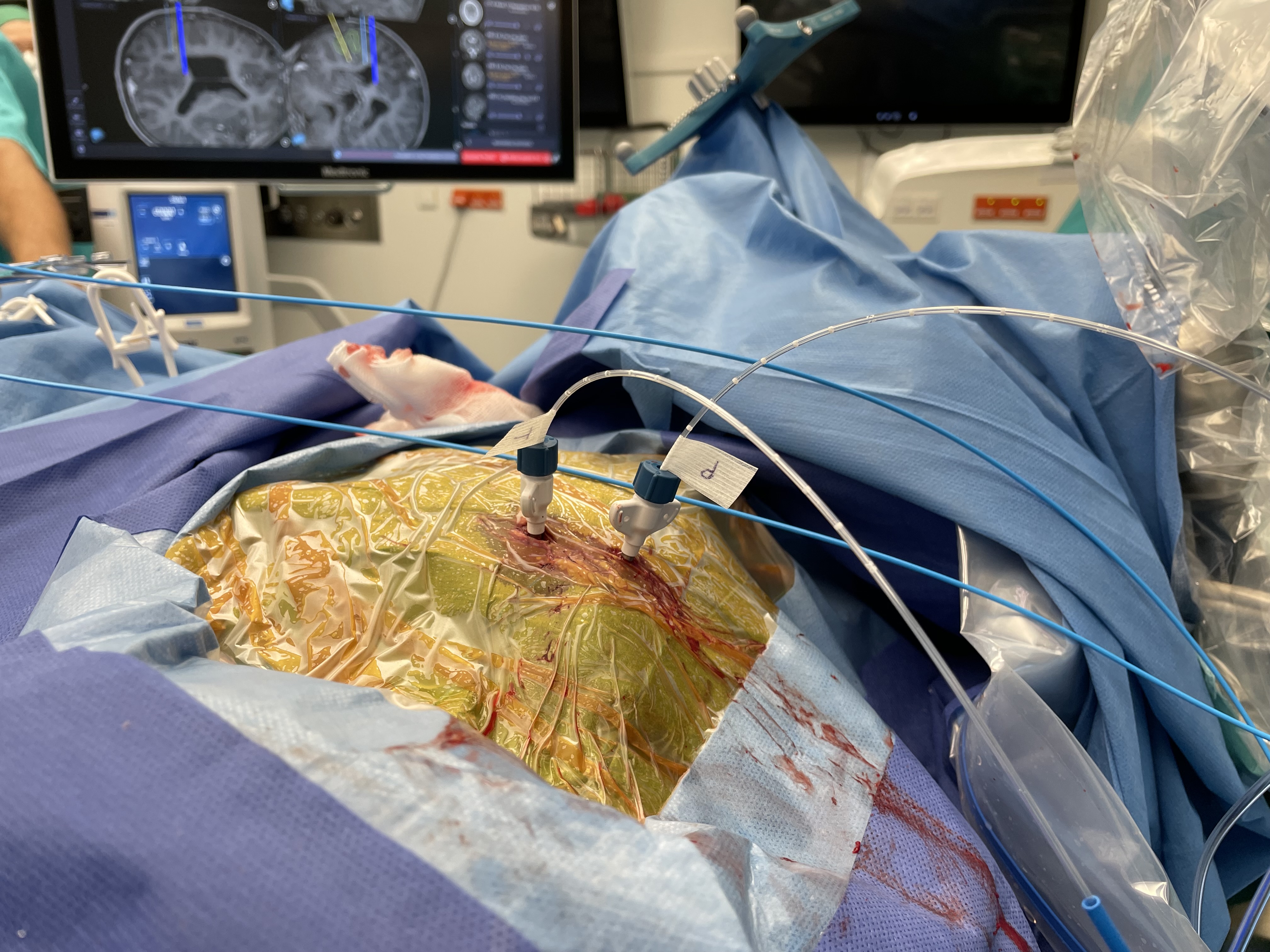
The Department of Neurosurgery at the Medical University of Vienna specializes in invasive cerebral epilepsy diagnostics (electrode implantations) in order to provide adequate evaluation and treatment even for patients with complex disease courses. For the treatment of medication-resistant epilepsy, vagus nerve stimulators have also been implanted.
An important aspect of epilepsy surgery is the planning and placement of electrodes for invasive EEG monitoring.
Through continuous optimization of multimodal imaging and the in-house development of a navigation-guided depth-electrode placement technique (Dorfer et al., Neurosurgery, 2014: Frameless Stereotactic Drilling for Placement of Depth Electrodes in Refractory Epilepsy: Operative Technique and Initial Experience), depth electrodes are increasingly being used compared with subdural electrodes in invasive diagnostics.
The most common epilepsy-surgical procedures at our clinic include, on the one hand, resections of epileptogenic lesions, such as low-grade tumors (LEATs) or focal cortical dysplasias, and on the other hand various techniques of temporal resection for temporal lobe epilepsy.
In severe pharmacoresistant forms of mesial temporal lobe epilepsy, amygdala-hippocampectomies are performed at our clinic, as well as anatomical perithalamic hemispherotomies, a procedure that, to date, is offered in Austria only at our clinic.
Disconnection refers to the separation of diseased, epileptogenic brain areas from the healthy brain without removing them. Through this procedure, the affected brain regions are electrically isolated from the rest of the brain.
A typical example of this non-resective surgical technique is the evolution from anatomical hemispherectomy—the complete removal of one cerebral hemisphere—to functional hemispherotomy, which involves functionally disconnecting one half of the brain without resecting the hemisphere.
In neurostimulation, pacemakers protect brain cells from abnormal electrical discharges.
After the procedure, four out of ten patients experience fewer epileptic seizures.
In epilepsy treatment, two types of pacemakers are distinguished:
- Vagus nerve stimulation: The pacemaker is placed on a nerve outside the brain. Since this nerve also contains fibers that run from the periphery to the brain, the pacemaker can influence brain cells.
- Deep brain stimulation: The pacemaker is located within the brain itself, where it directly influences brain cells.
Clinical Working Group for Epilepsy Surgery
Head:
Univ.-Prof. Dr.med.univ. Karl Rössler
Stv. Leitung:
PD DDr. Johannes Herta
