In line with the specialization of our clinic, surgical procedures for brain tumors are the most frequently performed operations
The use of modern molecular genetic analyses has revolutionized the diagnosis and treatment of brain tumors in recent years, enabling more precise diagnoses, better prognostic assessment, and optimization of postoperative therapy management in the context of precision medicine.
Through the Oncology Outpatient Clinic, highly specialized care for all epilepsy surgery patients is ensured, both preoperatively and during postoperative follow-up. Optimal patient care is further supported by close collaboration with other medical specialties within the framework of the Interdisciplinary Tumor Board and Pediatric Tumor Board, where an individualized treatment plan is developed.
Process of brain tumor treatment at our clinic:
Imaging diagnostics are essential as part of preoperative evaluation and surgical planning
To optimize and standardize preoperative evaluation, an MRI protocol was developed in cooperation with the University Clinic for Radiology and Nuclear Medicine. This protocol includes diagnostic imaging (MR spectroscopy, perfusion MRI, ASL, SWI), anatomical and metabolic imaging (MR spectroscopy), as well as functional imaging (fiber tractography, DTI). Additionally, positron emission tomography (PET) provides further metabolic information about the tumor and its activity. For tumors located near functional brain areas such as motor or language regions, functional MRI (fMRI) can visualize these areas, thereby optimizing preoperative surgical planning and increasing procedural safety.
Using image fusion, a patient-specific brain model is created from anatomical, functional, and metabolic imaging data. Mapping of functions to anatomical structures is performed through 2D and 3D representations of fMRI and tractography data of the brain surface. This allows the definition of the optimal surgical access path and enables surgical simulation during preoperative planning.
Close collaboration with the University Clinic for Neurology is particularly important in the preoperative evaluation of epileptic seizures and optimization of seizure management, as these are common symptoms of brain tumors.
Within clinical studies, additional imaging techniques such as high-field/7 Tesla MRI and specialized MRI sequences are frequently applied.
Neuronavigation is now an indispensable tool for tumor resections and biopsies
In the neuronavigation system and the neurosurgical microscope, preoperatively acquired imaging data are fused and integrated, ensuring maximum safety and precision during the procedure. In addition, intraoperative neurophysiological monitoring provides an additional technique for observing and preserving neurological functions during surgery.
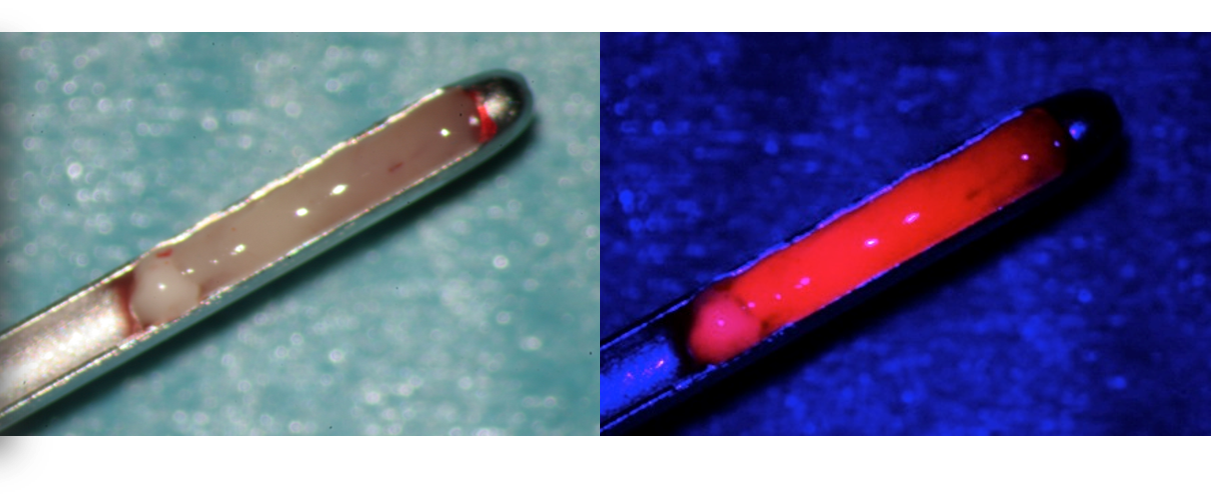
To achieve the goal of maximal tumor resection, since 2007, fluorescence technology with 5-aminolevulinic acid (5-ALA) has been used intraoperatively to improve visualization of tumor boundaries. This technique has proven essential not only for maximizing the resection of malignant gliomas but also for suspected low-grade gliomas and meningiomas.
Further optimization of brain tumor resection is made possible through the use of intraoperative MRI. This allows any residual tumor to be detected and removed during the operation. The use of this innovative technology increases the rate of maximally safe and, whenever possible, complete brain tumor resections, thereby improving the prognosis and therapeutic success.
After a brain tumor resection, patients are cared for postoperatively in our neurosurgical intensive care unit on level 11 or in the two bed wards on levels 9 and 10. To monitor the extent of tumor removal, patients with primary brain tumors and cerebral metastases typically undergo an early postoperative MRI. Following surgery, patients are discussed in the context of the Interdisciplinary Tumor Board to develop an individualized postoperative treatment plan.
Clinical Working Group for Neuro-Oncology
Head:
Assoc. Prof. Priv.-Doz. Dr.med.univ.et scient.med. Georg Widhalm
Deputy:
Dr. med.univ.et. scient.med Barbara Kiesel