Pituitary, the interface between the endocrine system and the nervous system
Transcranial operations for pituitary adenomas were already being performed at the end of the 19th century. Using the transsphenoidal approach, the Austrian ENT surgeon Hermann Schloffer successfully carried out the first removal of a pituitary adenoma in 1907. The introduction of the operating microscope and the image intensifier by Jules Hardy in 1963 marked further advances in pituitary adenoma surgery.
On the occasion of the 100th anniversary of the first transsphenoidal pituitary operation in 1907, the Vienna University Clinic for Neurosurgery hosted the meeting of the International Society of Pituitary Surgeons (ISPS) in 2007 at the Altes AKH in Vienna, attended by around 100 pituitary surgeons from all over the world.
Pituitary Surgery - Innovations in Surgical Techniques and Visualization
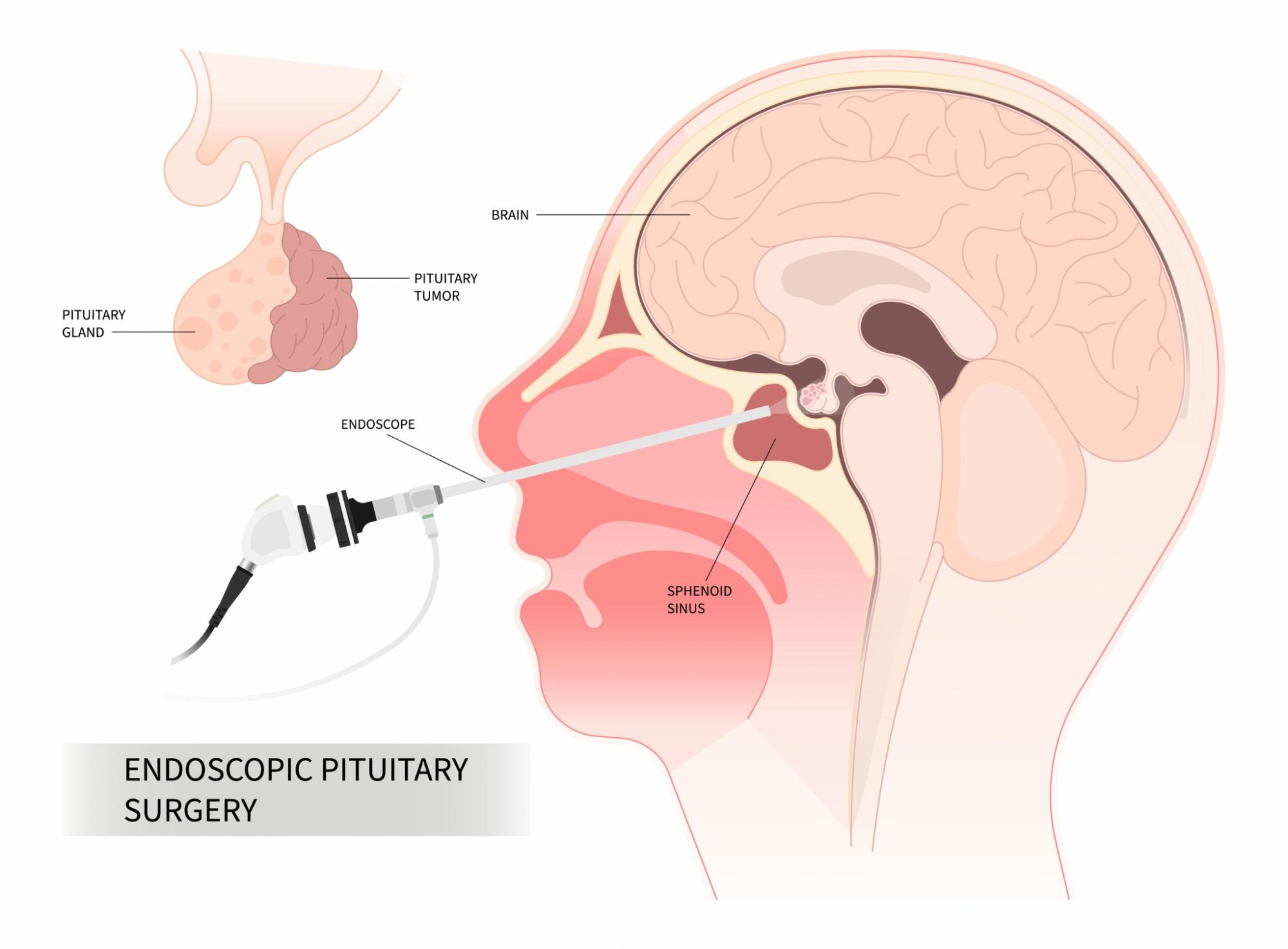
In 2002, endoscopic pituitary surgery was introduced at the Medical University of Vienna and the Vienna General Hospital Department of Neurosurgery, and it has since almost completely replaced the microscopic technique. Since then, more than 700 procedures have been performed purely endoscopically, via a transnasal and transsphenoidal approach. The initially mononostril approaches were further developed into binostril and “extended” approaches, enabling the purely endoscopic removal of lesions in the perisellar region (supradiaphragmatic, frontobasal, clival, etc.).
Through these advancements (instruments and increasing experience with endoscopic surgical techniques), so-called “extended approaches” now allow lesions in difficult-to-reach areas of the skull base to be operated on safely and efficiently. In particular, pathologies located along the midline—frontobasal, supradiaphragmatic, and clival—can be accessed endoscopically via a transnasal route.
Endoscopic imaging has also improved significantly since 2002: since 2019, a high-resolution 3D HD endoscope has been available, overcoming the previous disadvantage of endoscopy—namely its exclusively two-dimensional view—thereby improving orientation and making endoscopic procedures even safer.
A further improvement has been achieved through advances in imaging in cooperation with the Division of Neuroradiology and Musculoskeletal Radiology of the University Clinic of Radiology and Nuclear Medicine: with the MR pituitary protocol, special high-resolution imaging sequences are now available for intraoperative neuronavigation during endoscopic transsphenoidal procedures.
For training and surgical planning, a simulator for transsphenoidal endoscopic pituitary surgery (STEPS) was developed in 2004 in collaboration with TU Vienna and the Center for Virtual Reality and Visualization (VRVis). This allows the individual patient’s anatomy to be represented preoperatively in the endoscopically distorted view and anticipated in various scenarios. Further development of this simulator took place on two fronts: in Vienna, through intraoperative integration with navigation systems, and in Montreal, Canada, via an endoscope module in the NeuroTouch® simulator.
Clinical Working Group for Pituitary Surgery
Head:
Ao.Univ.-Prof. Dr.med.univ. Christian Matula
Deputy:
Priv.-Doz. Dr.med.univ. et scient.med. Matthias Millesi
