Spinal neurosurgery: microsurgery to prevent paraplegia
The University Clinic for Neurosurgery has made significant contributions to improving the treatment of patients with spinal disorders. New surgical techniques for the cervical spine have been developed and implemented, established procedures clinically evaluated, methodologies improved, and new implants tested and introduced.
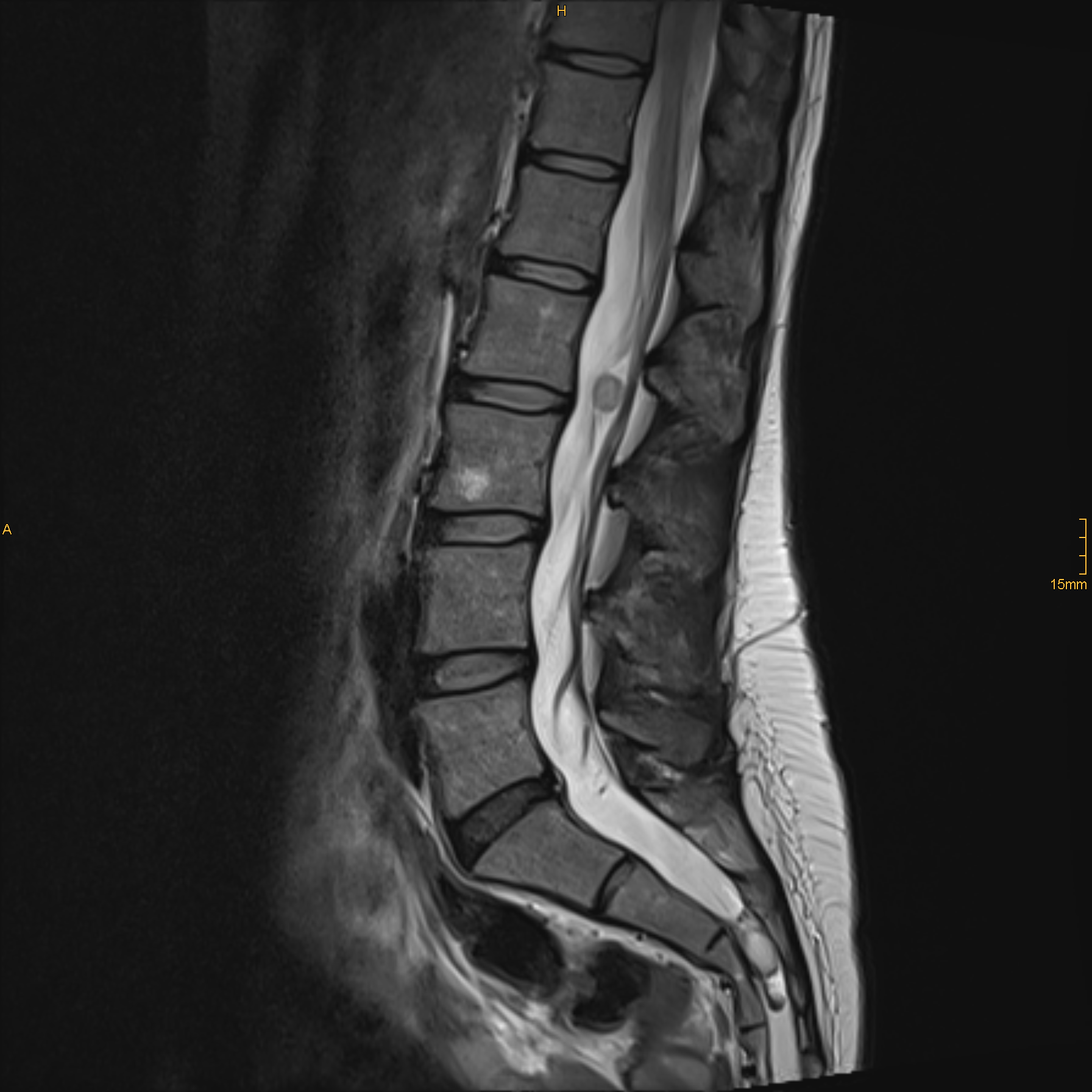
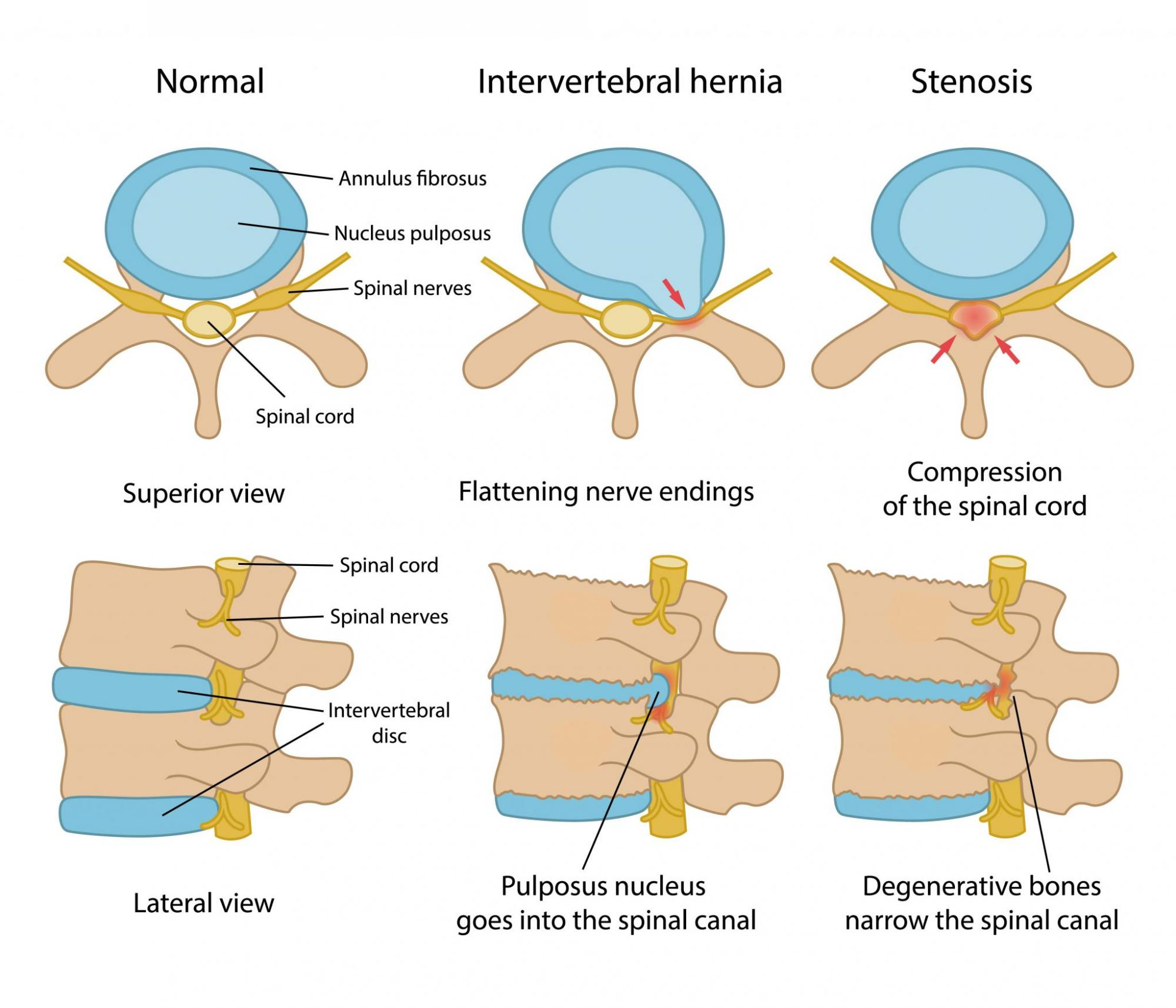
Surgical treatment—either microsurgical or endoscopic—is performed for all forms of degenerative spinal diseases, including herniated discs, vertebral stenoses, foraminal stenoses, Arnold-Chiari malformations and pseudospondylolisthesis, as well as extra-/intradural and intramedullary tumors such as schwannomas, ependymomas, meningiomas and gliomas.
For tumors in functionally critical locations, intraoperative neurophysiological monitoring is routinely used during surgery to supervise neurological function.
Individualized therapy concepts and strategies for patients treated at our clinic with spinal neurosurgical disorders are developed within the framework of the Spine Specialty Clinic and the interdisciplinary Spine Board.
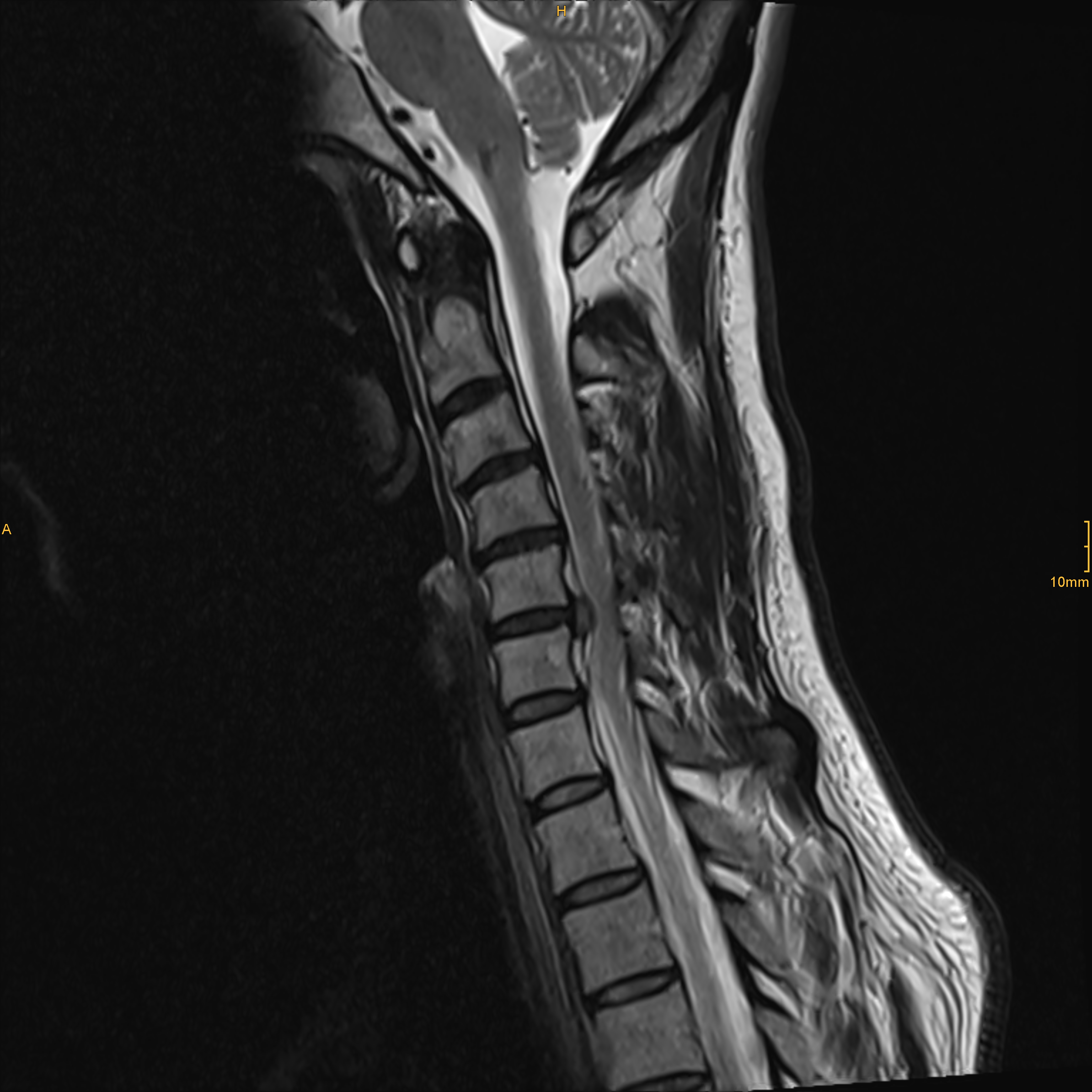
At the University Clinic for Neurosurgery, the main focus in the treatment of degenerative spinal diseases lies in the cervical spine.
In recent years, several types of cervical disc prostheses have been tested. Currently, a diamond-coated, biologically inert, and easy-to-implant prosthesis is used, which has demonstrated good long-term outcomes.
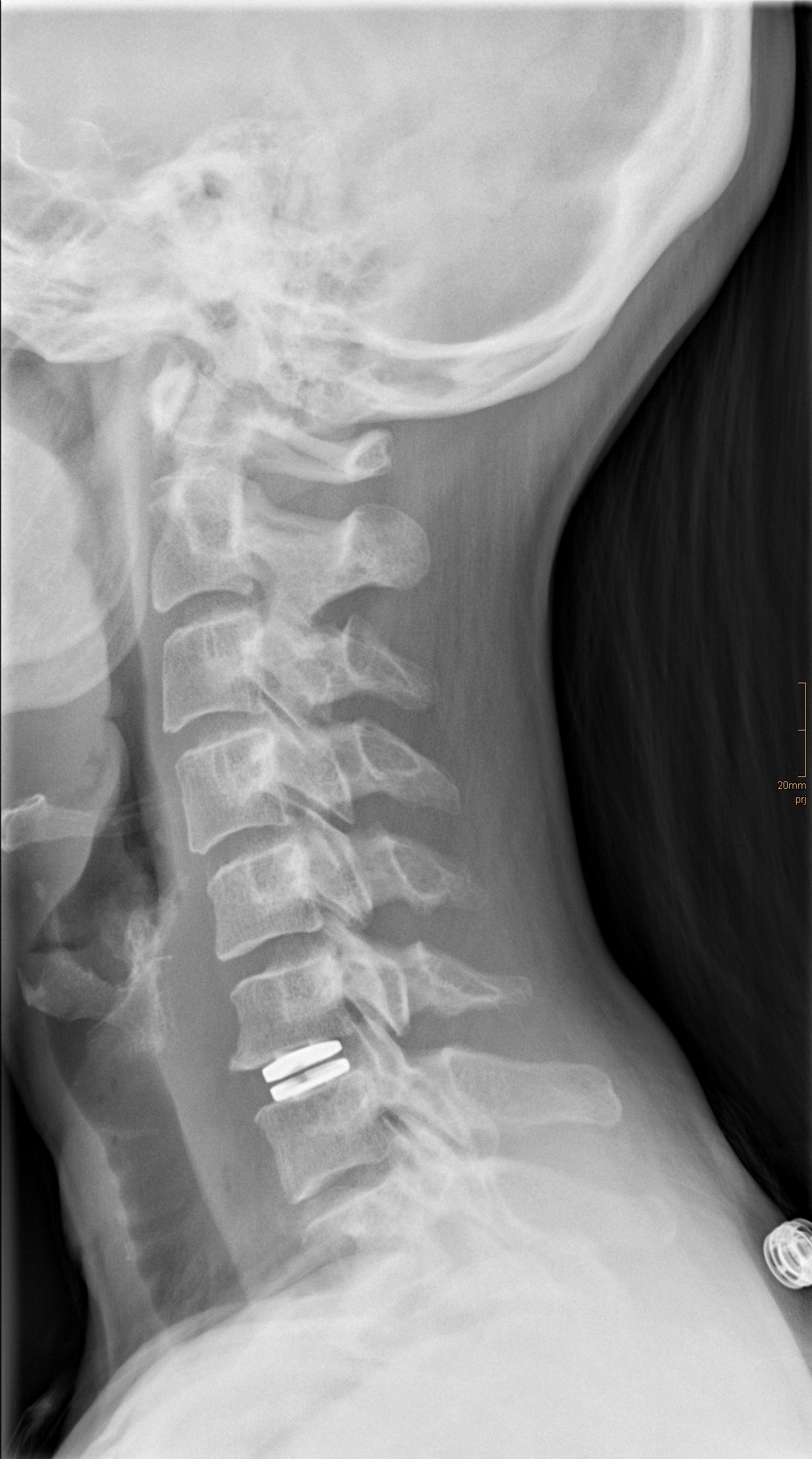
Ao.Univ.-Prof. Dr.med.univ. Walter Saringer developed and implemented a new surgical technique at the clinic for the treatment of foraminal stenosis and herniated cervical discs: the microsurgical and endoscopic ventral foraminotomy.
In the publication “Microsurgical anterior cervical foraminotomy (uncoforaminotomy) for unilateral radiculopathy: clinical results of a new technique” (Saringer et al.), this method is described in detail.
During this procedure, a small drill channel of about 5 mm is created from the ventral (anterior) side through the vertebral body into the neuroforamen. In contrast to the conventional anterior body fusion (ABF) technique, the uncoforaminotomy does not require complete removal of the intervertebral disc or implantation of a cage to fuse the spinal segment. Fusion procedures have the disadvantage of accelerating degenerative changes in adjacent segments. Uncoforaminotomy largely preserves the mobility and function of the operated segment.
The advantages of this technique compared with conventional surgical methods include the minimally invasive approach, the possibility of operating on several segments simultaneously, and the avoidance of spinal fusion. As a result, the mobility of the treated segments is maintained and adjacent segment disease—the premature degeneration of neighboring segments—can potentially be prevented.
Extradural, intradural, and intramedullary tumors of the spine—including schwannomas (neurinomas), ependymomas, meningiomas, gliomas, hemangioblastomas, and others—are treated surgically using microsurgical or endoscopic techniques.
During operations involving functionally critical tumor locations, intraoperative neurophysiological monitoring is routinely used to supervise and protect neurological function throughout the procedure.
Clinical Working Group for Spinal Neurosurgery
Head:
Dr.med.univ. Magnus Kueß